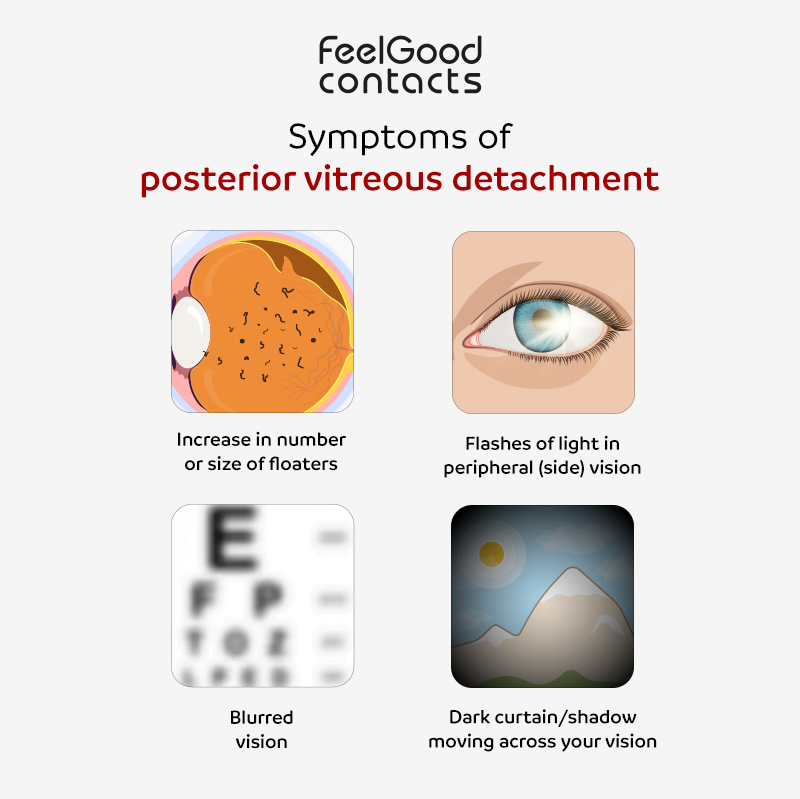
Symptoms of posterior vitreous detachment
Most people with PVD experience changes in their vision. However, the symptoms of a PVD can also be a sign that the retina has detached and requires urgent medical attention. It is not possible necessarily to distinguish the symptoms of a retinal detachment from a posterior vitreous detachment and any new PVD symptom should be checked by an eye physician promptly (< 24 hours). Here are some common symptoms:
Floaters
Floaters are small, moving spots that seem to float in your field of vision. They can look like tiny specks, strings or cobwebs. Although they are usually harmless, a sudden increase in their numbers or size could be a symptom of PVD.
Flashes of light
Sometimes, PVD can cause flashes of light in your vision. These flashes occur when the vitreous pulls on the retina. It’s similar to seeing stars after rubbing your eyes.
Blurred vision
Some people may also experience blurred vision as the vitreous detaches. This is often temporary and reduces as the eye adjusts.
A dark curtain over your vision
Seeing a dark curtain or shadow moving up, down or across your vision is a symptom of PVD.
Diagnosis of posterior vitreous detachment
Posterior vitreous detachment diagnosis involves a comprehensive eye examination by an ophthalmologist. They may perform a dilated eye exam to inspect the retina and vitreous gel. Optical coherence tomography (OCT) or ultrasound imaging can also be used to assess the condition of the vitreous and retina.
Treatment for PVD
In most cases, PVD doesn't require treatment as the symptoms tend to resolve over time. However, if the detachment leads to complications such as retinal tears, further intervention may be necessary. The most common treatments include:
Surgery
In rare instances where PVD causes significant problems, such as retinal detachment, surgical intervention may be required. Vitrectomy is a procedure used to remove the vitreous gel and repair the retina.
Laser treatment
Laser treatment can be recommended if PVD causes a retinal tear. The laser helps seal the tear and reduces the risk of it progressing to retinal detachment. This treatment is usually quick and helps prevent further damage.
When to see an optometrist?
If you experience sudden or persistent symptoms of posterior vitreous detachment, like an increase in floaters, flashes of light or a shadow in your vision, seek immediate medical attention. These could be signs of a retinal tear, which requires urgent treatment.
Difference between degenerative vitreous syndrome and PVD
While PVD and Degenerative Vitreous Syndrome (DVS) may seem similar as they both involve changes in vitreous gel, they are different. PVD is the natural separation of the vitreous from the retina, whereas DVS is a condition where the vitreous gel becomes liquefied and degenerates without necessarily detaching.
Tips to maintain your eye health
Maintaining overall eye health is key to managing PVD and preventing additional eye problems. Here are some tips for the same:
- Regular eye exams: Visit your eye specialist regularly to monitor your eye health.
- Healthy diet: Consume foods rich in vitamins C and E, lutein and omega-3 fatty acids, all of which support eye health.
- Protect your eyes: Wear sunglasses to protect against UV light and safety glasses during activities that could potentially injure your eyes.
Frequently Asked Questions
Does posterior vitreous detachment (PVD) lead to vision loss?
Posterior vitreous detachment does not cause permanent loss of vision. However, any sudden increase in floaters or flashes should be checked by an optometrist.
Can I do anything at home to reduce floaters and flashes?
There is no treatment at home to stop floaters and flashing lights. In most cases, they become less noticeable over time.
How serious is posterior vitreous detachment?
PVD is usually a normal change that happens with age and is not serious. Regular eye examinations are important to prevent any related retinal problems.
What triggers vitreous detachment?
Vitreous detachment is mainly caused by age-related changes in the eye. It may also occur earlier in people who are short-sighted or have had eye injury or surgery.
What’s the difference between retinal detachment vs PVD?
PVD happens when the vitreous gel pulls away from the back of the eye and is usually not serious. Retinal detachment is when the retina itself separates from the eye and needs urgent medical treatment.
Disclaimer: The advice in this article is for informational purposes only and does not replace medical care or an in-person check-up. Please check with an eyecare professional before purchasing any products or remedies. For information on our article review process, please refer to our Editorial Policy.

 Offers
Offers Account
Account
 Favorite
Favorite
 Basket
Basket

 OFFERS
OFFERS